AI
Smart systems,
human decisions
Our platform is thoughtful about helping behavioral health providers do as much as humanly possible. We use AI to take the operational burden off your plate, so you can do good and do well.
OUR APPROACH
We're being intentional,
because we know what’s at stake
The use of AI in behavioral health comes with a healthy dose of skepticism. We get it. Patient care depends on human judgment and clinical expertise, and the last thing providers need is another tool that makes promises it can't keep.
That's why we don't use AI to replace your voice or your clinical intuition. We use it very intentionally to protect your effort to do good and do well. This is about being proactive — catching billing risks or documentation gaps before they become problems — and helping your practice become more efficient, audit-ready, and financially resilient.
Everything we've built follows one principle: you stay in control.
BEHAVIORAL HEALTH-SPECIFIC
Built for the workflows and complexities that matter most in your practice
We're not using AI for the sake of AI. Every feature below was designed to solve a specific problem behavioral health practices face every day: staying compliant, reducing claim denials, and giving providers more time for patient care. This is AI that does the detail work, so your team can focus on what actually matters.
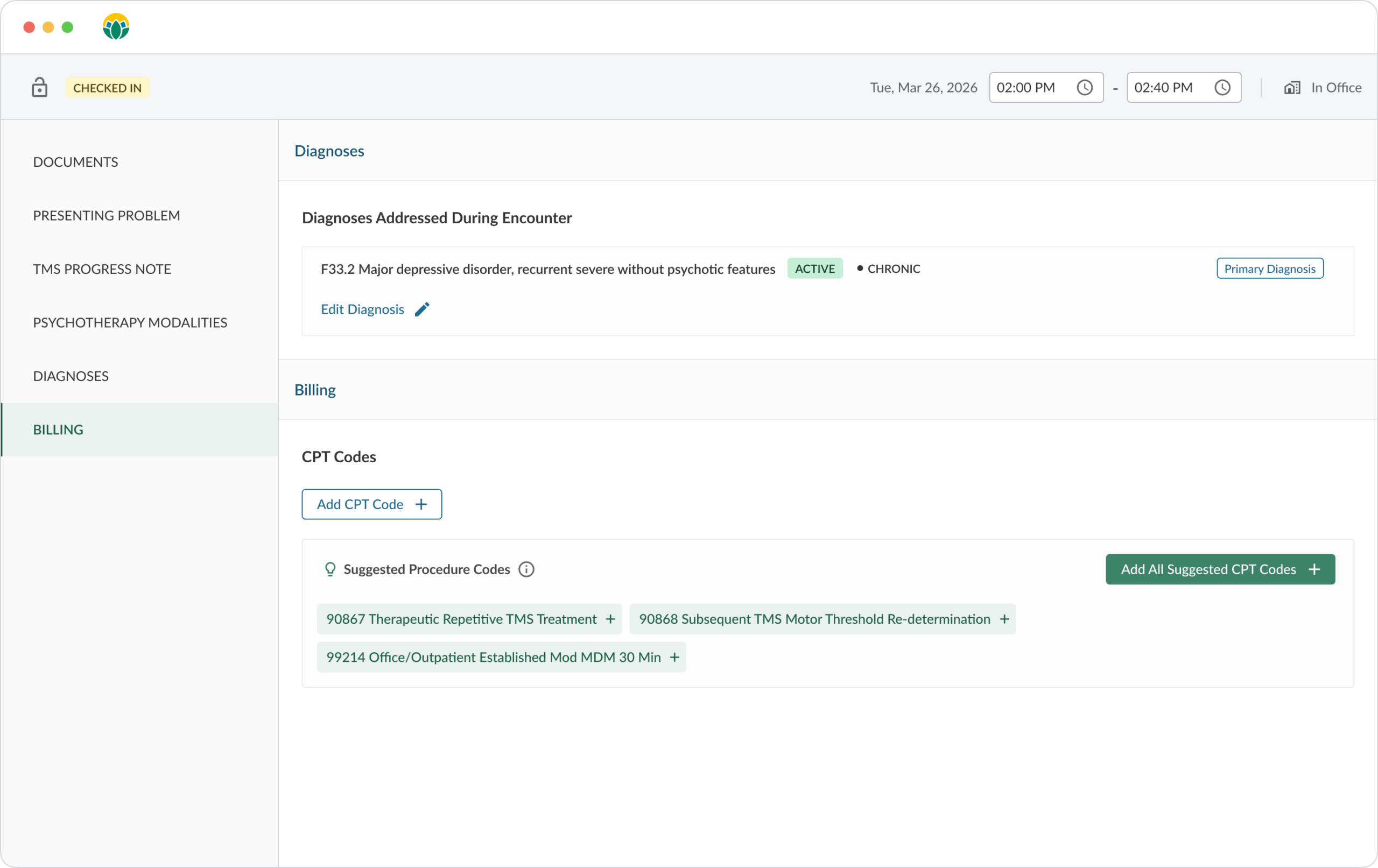
Coding assistant
CLINICAL SUPPORTWhen a provider documents a session, the system analyzes the note and suggests the appropriate CPT codes based on rules your administrators have configured. The provider reviews and confirms.
Why it matters: No more searching through thousands of codes or second-guessing whether you picked the right one. Accurate coding from the start means faster reimbursement, fewer denials, and a built-in learning tool for newer clinicians on your team.
Medication interaction management
CLINICAL SUPPORTWhen a prescription or diagnosis is updated, the system automatically checks for drug-to-drug and drug-to-allergy interactions and flags potential risks before anything is finalized.
Why it matters: Providers get real-time clinical decision support at the point of care, which helps prevent adverse events and keeps medication management both efficient and safe.
Documentation alerts
CLINICAL SUPPORTThe system monitors notes for missing details that could create compliance risks or billing denials (e.g, missing time stamps, incomplete risk assessments, or unsigned documents) and alerts the provider before the note is finalized.
Why it matters: Clinicians can finish their documentation right the first time, which means fewer back-and-forth requests from billing, cleaner audit trails, and notes that are always ready for payer review.
Compliance monitoring
OPERATIONAL SUPPORTThe system tracks treatment plan renewal dates, credential expiration timelines, and authorization limits, and alerts the responsible team member when deadlines are approaching.
Why it matters: Compliance stays on track without someone manually monitoring a spreadsheet. Your team gets notified before something becomes a problem, not after.
Automated task management
OPERATIONAL SUPPORTWhen specific events happen in a patient's care journey — like a new intake is completed, a supervisor review is needed, or an authorization is approaching its limit — the system automatically assigns tasks to the right team member based on rules you've configured.
Why it matters: Clinical and administrative work flows to the right person without manual coordination. Intake coordinators, supervisors, and billing staff stay on top of their responsibilities.
Revenue risk detection
FINANCIAL SUPPORTThe system scans for unbilled visits, expiring prior authorizations, and missing claim modifiers, and routes issues to your billing team with context already attached.
Why it matters: You catch revenue leaks before they become write-offs. Every flagged unbilled visit or expiring authorization is money your practice would have otherwise lost.
Automated claims scrubbing
FINANCIAL SUPPORTBefore a claim leaves your system, the system scans it for payer-specific errors, common submission mistakes, and missing information. Issues get flagged for review or corrected automatically, depending on how you've configured the system.
Why it matters: Fewer denials. Faster reimbursement. Clean claims get paid correctly the first time, which means less time spent on appeals and rework.
HUMAN-IN-THE-LOOP
Total clinical autonomy, zero guesswork
We believe AI in healthcare should support decision makers, not be a decision maker. That's why we built ProsperityEHR with a human-in-the-loop architecture. You're the expert in the room, and our AI acts as a sophisticated safety net. It flags potential billing errors or clinical risks in real time, but it never acts without you.

FAQs
Common questions about ProsperityEHR and AI in behavioral health tech
See how reactive AI can help your practice stay sustainable
without compromising on the human touch